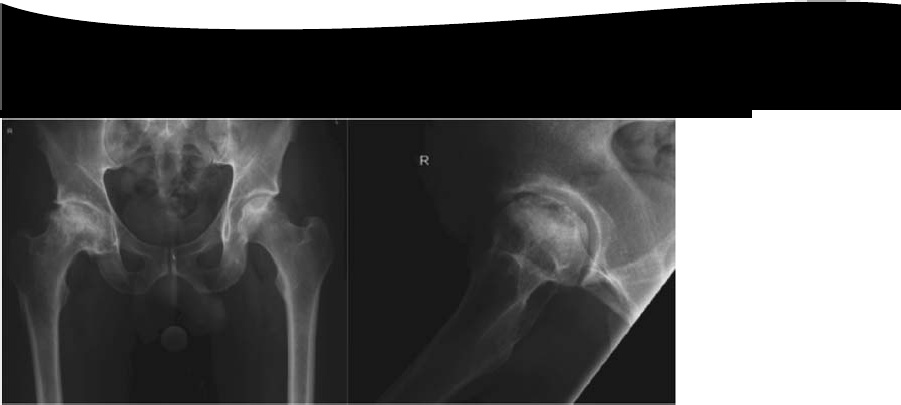
Avascular necrosis of the femoral head with segmental collapse.
Osteonecrosis (avascular necrosis/aseptic necrosis) occurs within the bone following loss of osseous blood supply. All cells within the area of affected bone die away; initially the organic and inorganic matrix are unaffected. It commonly affects patients in the third, fourth, or fifth decades of life.
The aetiology of osteonecrosis is still not fully understood and is likely to be multifactorial.
Factors thought to contribute to the disruption of the microcirculation include:
Trauma —leading to macro- and microvascular interruption
Intravascular coagulation and thrombotic occlusion of microcirculation
Extravascular compression (‘compartment syndrome’ within bone) secondary to raised intra-osseous pressures
Conditions associated with osteonecrosis include:
Trauma
Caisson disease (dysbaric osteonecrosis)
High alcohol intake
Systemic lupus erythematosus (SLE)
Corticosteroid usage
Ionizing radiation
Haemoglobinopathy (sickle cell anaemia)
Gaucher’s disease
Hypercoagulation disorders
Idiopathic (40%)
Other areas most commonly affected are:
medial femoral condyle;
humeral head;
talus;
lunate(Kienböck’s disease);
capitellum (Panner’s disease);
tarsal navicular (Kohler’s disease);
metatarsal head(Freiberg’s disease).
There are many classification systems described for osteonecrosis of the hip.
The Ficat and Arlet(1980) system describes X-ray appearances and is one of the most simple to use:
Stage 1: no bony changes seen on plain X-ray
Stage 2: sclerotic and cystic changes within the femoral head
Stage 3: subchondral collapse and distortion of the femoral head
Stage 4: secondary osteoarthritis with decreased joint space and articular collapse
The radiographs show Ficat and Arlet stage 4 changes. There is distortion and collapse of the femoral head. The lateral view illustrates the ‘crescent sign’ associated with subchondral collapse.
Treatment of early osteonecrosis of the femoral head aims to relieve pain and preserve the congru-ency of the hip joint. In the later stages of the disease arthroplasty procedures are usually required.Investigations used to help stage the disease include plain radiography, bone scans, and MRI.
Treatment for early stages (pre-collapse) may include:
Observation and analgesia
Treatment of any underlying medical conditions
Protected weight-bearing (little evidence)
Core decompression ± bone grafting or vascularized grafts
Treatment for later stages (post-collapse) may include:
Realignment osteotomy
Arthrodesis
Replacement arthroplasty (conventional total hip arthroplasty or resurfacing)
Leave a Reply